Last week, a young man walked into Dev’s Oral Care with his mother. He was 24, preparing for his MBA entrance exams, and had been managing what he thought was “just a wisdom tooth problem” for close to two months.
He had finished two courses of antibiotics. The swelling had reduced both times. He had been telling himself and his mother that it was settling down.
It wasn’t.
By the time he came in, the infection had involved the tissue beyond the tooth, his jaw was partially stiff, and the second molar next to the wisdom tooth had already begun to show changes on imaging.
He didn’t ignore the infection because he was careless. He ignored it because it kept appearing to get better.
That is exactly what makes wisdom tooth infections tricky and exactly what this blog is about.
I understand why patients delay.
The pain peaks for a few days, you take antibiotics, the swelling reduces, and life goes back to normal. Exams are coming. There’s a function in the family. Work can’t be put on hold right now. And honestly, if the pain is manageable again, why rush into something that might involve surgery?
This is a completely rational way of thinking.
The problem is that the infection is not following the same logic.
Here’s the part most patients don’t fully understand.
Antibiotics reduce the bacterial activity in the area. Painkillers suppress the signal. Rest reduces the swelling. But none of these treatments removes what created the infection in the first place.
If your wisdom tooth is partially erupted, meaning it has only come through the gum partially, there is a flap of gum tissue sitting over it. Food, bacteria, and debris collect underneath that flap every single day. No amount of rinsing or medication eliminates that environment.
So the infection clears temporarily. And then it returns.
Each time it returns, the surrounding tissue is a little more damaged than before. The body’s ability to fight it off becomes a little less efficient. And your options for simple management begin to narrow.
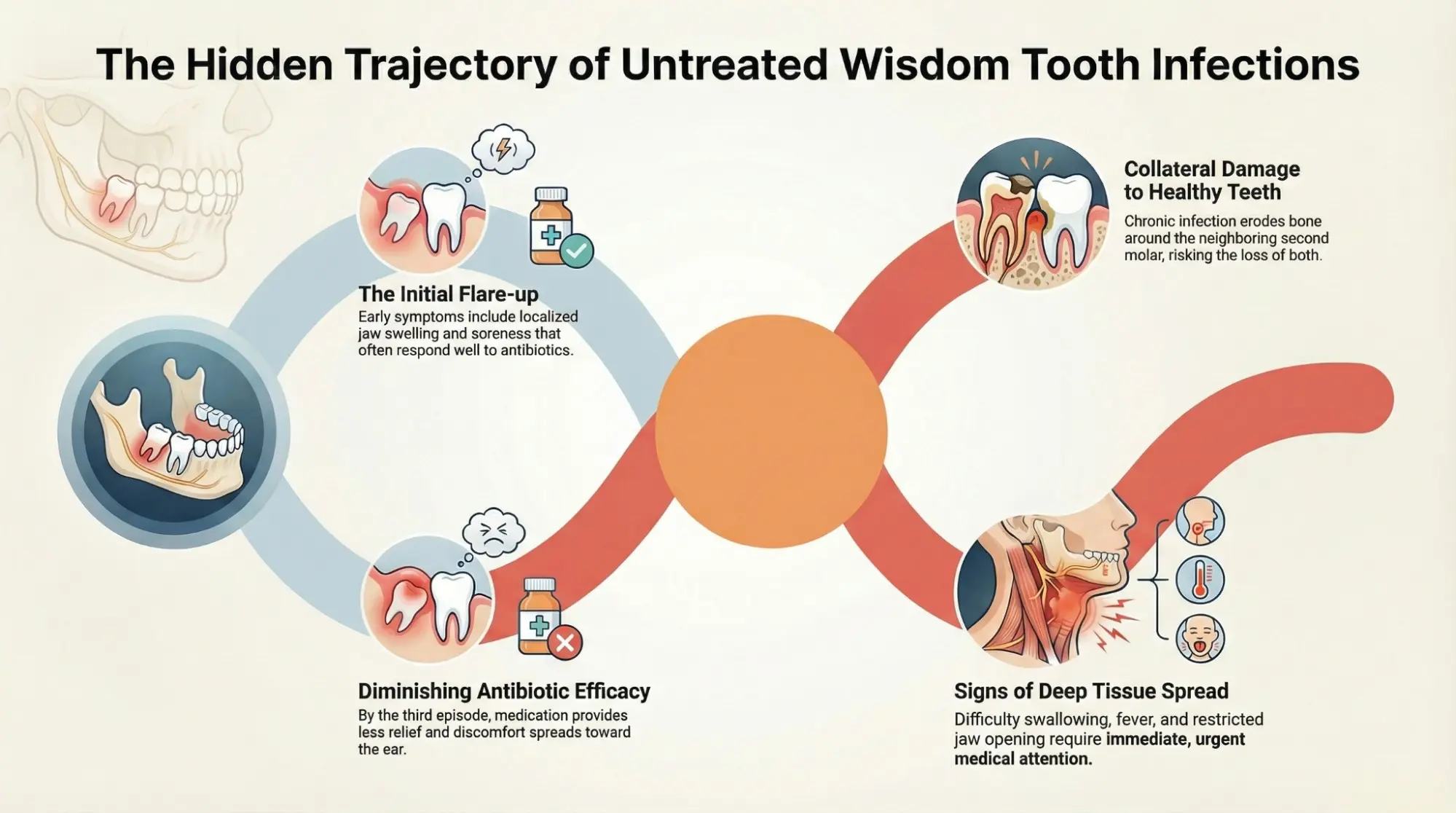
I’m not going to describe rare complications or worst-case scenarios. What I want to share is what I actually see in practice, the realistic trajectory when infections are left unmanaged over weeks and months.
Localised swelling near the back of the jaw. Soreness while chewing. Some stiffness in the morning. A bad taste that comes and goes. Most patients handle this with antibiotics and assume the problem is resolved.
The response to antibiotics feels less complete. The swelling takes longer to reduce. The discomfort sometimes spreads slightly along the jaw, sometimes toward the ear or throat. Patients start to notice it’s taking more medication to get the same relief.
This is the part that surprises patients most. The tooth sitting right in front of the wisdom tooth, usually the second molar, is under continuous stress when there is chronic infection nearby. The bone around its root begins to erode quietly. By the time this shows up on an X-ray, it often needs treatment of its own.
Ignoring a wisdom tooth infection can end up costing you the tooth next to it. That is the realistic consequence I see most often not the dramatic stories, but this quiet, preventable damage to a perfectly healthy neighbouring tooth.
If the infection moves beyond the tooth and surrounding gum tissue into the deeper tissue spaces of the jaw, the nature of the problem changes significantly. This is not common, but it is also not rare when infections are repeatedly suppressed without proper management.
Signs that this may be happening: difficulty swallowing saliva, visible swelling along the jaw or under the chin, the inability to open your mouth fully, or fever alongside facial swelling. These are not signs to observe at home. These require urgent attention.
One of the most common things I hear: “Doctor, antibiotics always work for me. Why do I need anything else?”
Antibiotics work on the bacteria. They do not work on the cause.
Think of it this way: if water is leaking through a crack in your wall, you can keep mopping the floor. The floor looks dry. The problem appears resolved. But the crack is still there, and the water keeps coming.
That is what repeated courses of antibiotics without source control look like. You are managing symptoms, not addressing the reason the infection keeps returning.
Over time, repeated antibiotic use also carries its own consequences, changes in your gut health, and, in some cases, reduced effectiveness against the same bacterial strains.
“The swelling is gone now. Can I wait a bit longer before deciding?”
You can. But understand that the window of simple management gets smaller with each episode. A case that is straightforward in the second episode often becomes more complex by the fourth. The decision doesn’t have to happen during an acute flare; in fact, it’s better made between episodes, calmly, with proper imaging.
“Does every infected wisdom tooth eventually need to be removed?”
Not always. Some wisdom teeth can be managed if they are fully erupted, properly positioned, and genuinely accessible for cleaning. But partially erupted wisdom teeth with recurrent infections rarely remain stable in the long term. The gum flap does not go away on its own. This is something that can be assessed clearly with an X-ray and a proper evaluation, not something to guess at from home.
“What if I just keep managing it with medication?”
Every time you suppress the infection, you are borrowing time. That is not always wrong; timing matters, and sometimes waiting a few weeks is reasonable. But repeatedly borrowing time without a plan is what leads to the molar damage I described earlier. The difference between a reasonable delay and a costly one is whether you have a clear understanding of what’s happening and a plan in place.
If you’re reading this because something is going on with your wisdom tooth, I want you to come in before the next flare not in the middle of it.
In the middle of an acute infection, options are limited. We manage the pain, reduce the infection, and wait for things to settle before any further assessment is possible.
Between episodes, we can actually look at what’s happening. A proper X-ray tells us the position of the tooth, what’s happening to the bone around it, whether the neighbouring molar is being affected, and what the realistic path forward looks like. That information changes everything.
At Dev’s Oral Care, we don’t push you toward any particular decision. We show you what’s actually there and help you understand your options clearly. Sometimes that’s monitoring. Sometimes that’s a straightforward tooth extraction. Sometimes it’s more involved but far less involved than it would have been if the same situation had been left for another six months.
The cost of waiting isn’t always immediate. But it is always real.
If you’ve had more than one episode, or if something doesn’t feel right even after your last course of antibiotics, come in. Let’s take a proper look. That’s the right place to start.
Common wisdom tooth infection symptoms include pain at the back of the mouth, swollen or red gums around the wisdom tooth, jaw stiffness, and a bad taste or foul smell. Other signs may include pain while chewing, pus near the gum flap, or swelling along the jaw. A dentist usually confirms an infected wisdom tooth with a clinical exam and dental X-ray.
A wisdom tooth infection can spread within a few days to a few weeks if the source of infection is not treated. It may begin in the gum around a partially erupted tooth, but can extend to nearby tissues or the neighbouring molar. Warning signs of spread include facial swelling, fever, difficulty swallowing, or limited mouth opening.
Early symptoms of wisdom tooth infection include mild pain at the back of the jaw, swollen gums around the tooth, pain when chewing, and a bad taste in the mouth. These symptoms may temporarily improve with medication, but the infection often returns if the tooth is partially erupted.
If extraction is recommended, follow proper aftercare to prevent complications. Read the dos and don’ts after wisdom tooth extraction for guidance on safe recovery.